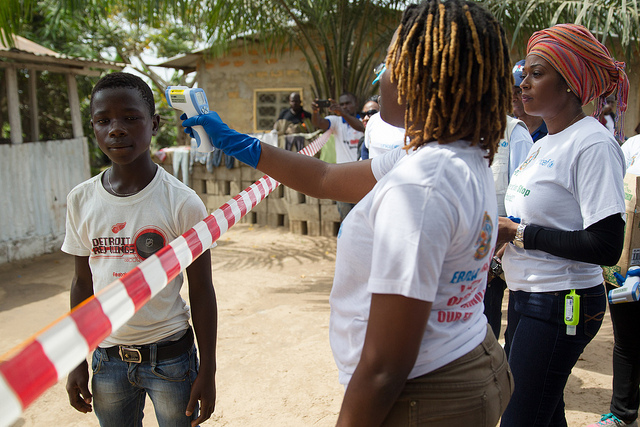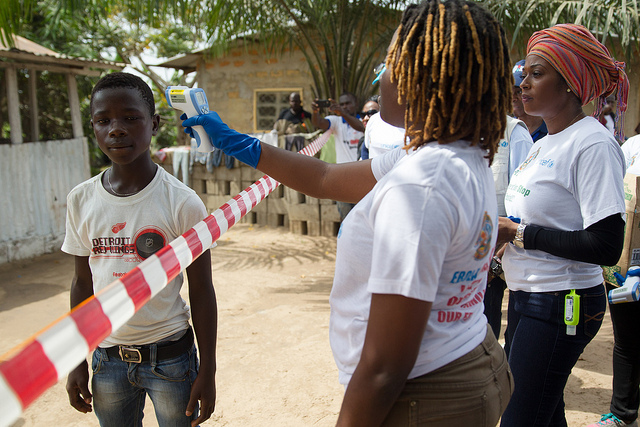
Image from the Flickr account of UNMEER.
By Arvind Badrinarayanan
The connection between conflict and health is well documented, whether it is the resurgence of Polio in vaccine-deprived Afghanistan and Syria, or traces of Uranium found in the parents of children suffering from congenital disease in Iraq. But rarely is the topic of iatrogenesis raised, even as healthcare workers travel worldwide, filling gaps in heavily burdened systems. From the ancient Greek, iatrogenesis refers to that which is brought forth by the healer. It may refer to anything from a mundane surgical scar to a hospital acquired antibiotic-resistant infection. The challenge today is to define such a term in the context of a global healthcare system where, from the hospitals of the developed world to the medical charities of the developing world, there is a multinational (read: biological) melting pot of professionals seeking the best opportunities available to them.
Nearly 700 years ago, the Mongol Khan Jani Beg, his own army weakened by disease, catapulted the deceased diseased into a besieged Crimean port. This primitive biological warfare partly led to the first pandemic of plague in Europe, spread by Genoan traders infected in Crimea fleeing through Europe. The Mongols were originally infected during their campaign in China, where the disease caused its most recent pandemic in the 19th century, emerging from the midst of the bloody Panthay revolution. The Mongol armies then brought it with them, infecting all the civilizations along the silk route, decimating their populations. Pillars of ancient civilization such as India, Byzantium, Egypt, Persia, and Greece, were depopulated in a couple of decades. Jews, pilgrims, beggars, lepers, Romani, and other minorities of Europe were slaughtered either by official sanction or by angry mobs. The Jewish population of Europe, isolated and confined to the ghettos, escaped major contact with the plague—and, for the same reason, were persecuted as its perpetrators. Over 500 Jewish communities in Europe, some numbering nearly a thousand people, were destroyed entirely. Some of the largest communities in Strasbourg and Basel were burnt alive, in the latter over 600 people, like a gruesome Viking funeral on the Rhine.
Veterinarians and other rural health workers are increasingly on the front lines of emerging diseases, and these are front lines drawn across the borders of nations globally.
Raised as an expatriate in the Arabian Gulf, I was familiar with this system and took advantage of it, volunteering to work with wildlife in diverse ecosystems from Central African banana republics to Southeast Asian tourist getaways. In hindsight, I had the potential to be a carrier for diseases, such as Newcastle’s disease from an Arabian Saker Falcon, or Tuberculosis from Asian Elephants. Though modern, and particularly medical, hygiene standards have dramatically cut the risk of this happening, it is only a matter of time before our idea of hygiene has to change to accommodate diseases fiercely evolving for survival.
On the shores of western Cameroon, back in 2007, I watched incredulous and impressed as a wildlife veterinarian tried and failed to orally resuscitate a young monkey dying of tetanus. Its tiny simian body was already curled with jaws clenched, “classical” as the veterinary manual says. But I was only partially in awe at the vet’s dedication to saving a life; there are a number of diseases which could have been transmitted in the process, putting his own life at risk. Although the world outside central and West Africa had largely forgotten about the existence of Ebola, it was a primary and constant source of concern when working with primates. Several of the major outbreaks since the discovery of the disease had taken place nearby, in the Democratic Republic of Congo, which was separated narrowly from Cameroon by the Republic of the Congo. Many of these are blamed on the bushmeat trade, responsible not only for the impending extinction of our fellow Homininae and other mammals, but also a primary disease feeder into our increasingly global populations.
Seven years later and many nations further west, crippled healthcare systems such as Liberia (fifty doctors for 6 million people) buckled under the pressure of an Ebola epidemic that went unidentified in neighboring Guinea for over five months. Vast colonies of bats, now known as the primary carrier of the Ebola virus, share nearly contiguous territories across sub-Saharan Africa. And although fruit bats remain among the most popular type of bushmeat, direct consumption is only one of a multitude of paths that could have led to the 2014 Ebola outbreak. Veterinarians and other rural health workers are increasingly on the front lines of emerging diseases, and these are front lines drawn across the borders of nations globally. Scarce news that emerges from conflict zones around the world is often a monocular lens to view the region.
It became natural to associate the disease with everything foreign and to assume that it was a deliberate infection of abandoned nations by the outside world.
In such a context, the universal outrage to condemn the Chibok kidnapping by Boko Haram came in the midst of the panic around Ebola. This took the focus temporarily off the spectacle of the lethal epidemic and the methods many countries globally were using to prevent, treat, and control the disease. Borders were closed and flights from affected regions canceled, and while this may have been ephemerally prudent, a darker culture of ignorance was floating around its incidence. Healthcare workers were treated with suspicion, their own strict quarantine procedures isolating them from their patients, emotionally and culturally. Their alien appearance, latex-wrapped hands reaching to take family members away into clinics, many never to be seen again, did not compute.
It was tougher still to understand in West Africa, where many cultures celebrate “standing by,” touching, kissing, hugging, washing the diseased and even the dead. Entire families dying, standing by one another, here where the mistrust of foreigners runs deep, where rich locals and white aid workers are flown out when infected, where local doctors die; it became natural to associate the disease with everything foreign, and to assume that it was a deliberate infection (if it was real at all) of abandoned nations by the outside world. The peak of suspicion in Guinea led to riots when teams in Hazmat suits descended to disinfect a market, which resulted in the murder of eight healthcare workers by a mob of crudely armed villagers. Where trust in healthcare and the government broke down, music provided a bridge of information to isolated villages over the radio. On the other side of the Atlantic as well, the Governors of New York and New Jersey united in their disagreement with the recommended quarantine procedures set by the Centers for Disease Control and Prevention (CDC). Their decades of scientific research on epidemic disease were abandoned by a few state governments in favor of excessive protocols that more often than not applied to the same medical personnel who risked their lives to control the outbreak.
The illusion of our invincibility by isolation persists.
The interface that global society has with disease is far greater than we care to imagine, where geographical boundaries are entirely irrelevant and political boundaries nearly so. We need to build strong medical and veterinary institutions locally with global links between them to be able to handle a crisis. But many governments prefer to pay for more powerful weapons to defend them from without while their bodies waste from within. India and Pakistan use 20 percent or more of their budgets on defense spending, but less than 4 percent is allocated to their healthcare budgets. Barbed wire borders, army platoons patrolling those perimeters, and satellites which can sense the spreading sickness take priority over healthcare education and affordable disease diagnostics. Medical tools such as isolation (of sick patients) and quarantine (of the potentially infected) are now political weapons. The word “quarantine” itself comes from quaranta giorni, the forty days one would have to remain on board before being allowed to dock in many European ports during the Bubonic Plague epidemic. Nothing, however, stopped the disease-carrying fleas as their rodent hosts swam ashore.
We forget that even our minutest of enemies and their hosts will fight at every turn for life, despite the willpower of mankind against them. The illusion of our invincibility by isolation persists, despite the number and diversity of animal hosts. Many of these animals, wildlife in particular, are not monitored; their roles as reservoirs for many deadly diseases are poorly understood. In itself, disease can be considered a failure on the part of the causative organism unable to live within its host without self-destructively killing it. The most successful, highly evolved organisms are the billions that live peaceably within their hosts, forming the local “biota.” These not only tend to outnumber the host’s native cells in quantity but form an integral part of protection against a wide variety of diseases. Information about the diversity of human bodies and their biota is therefore as vital as information about the disease in this conflict.
Vaccines, to use a topical metaphor, can be considered “information” given to the immune system, a biological spy leaking virulent secrets to the security apparatus of the body. Human medicine driven by consumption prefers the traditional ammunition of antibiotics that can affect short term victories in a “shock and awe” campaign, but conversely, provides the surviving enemy with extensive information about our weaponry. And, similarly to traditional weaponry, there is substantial collateral damage, particularly to one’s own biota; there is also a highly profitable economic model of repeated consumption that this allows. Veterinary medicine however, driven by cost efficiency, has experienced a tremendous revolution in vaccine availability, cost, and efficacy. Similarly, in countries where the cost of vaccine development or its subsequent financial returns is not viewed as important as its overall efficacy, several innovations have left the developed world far behind. Cuba today produces a vaccine for lung cancer, veterinarians have had a more cost-effective rabies vaccine for decades, and by 2010 India was producing 60 percent of the world’s vaccines.
Sun Tzu’s Art of War gives us an answer with a similar ideology:
“So it is said that if you know your enemies and know yourself, you can win a hundred battles without a single loss.
If you only know yourself, but not your opponent, you may win or may lose.
If you know neither yourself nor your enemy, you will always endanger yourself.”
In times of conflict, the breakdown of healthcare and its supply chains can make it hard to actively combat emerging diseases. Protracted conflicts create geographical zones where the lack of prophylaxis allows easily preventable conditions to re-emerge and spread. The diagnosis, prevention, and treatment of disease are traditionally dependent on highly centralized facilities with large scale processes to minimize costs. Technology available today, however, can bring both cost-effective diagnostics and high quality vaccine manufacturing to where it should always have been—with local healthcare institutions that can provide both support and education to the communities they serve.
As a veterinarian, I have observed that funding for technology development and commercialization mostly targets the medical needs of high-income patients. I felt then the need to not just build devices and diagnostic solutions but to begin an approach that views the healthcare worker whose services reach the most marginalized as our primary customer and their local community as our supplier. Additionally, this will result in upending the traditional dynamics of production through distributive manufacturing and assembly while producing innovations that can rapidly decentralize medicine. Only when this kind of a revolution happens can we begin to see an end to our conflict with disease.